Surgical Procedures: Surgery and Staging for Parathyroid Cancer
Table of Contents
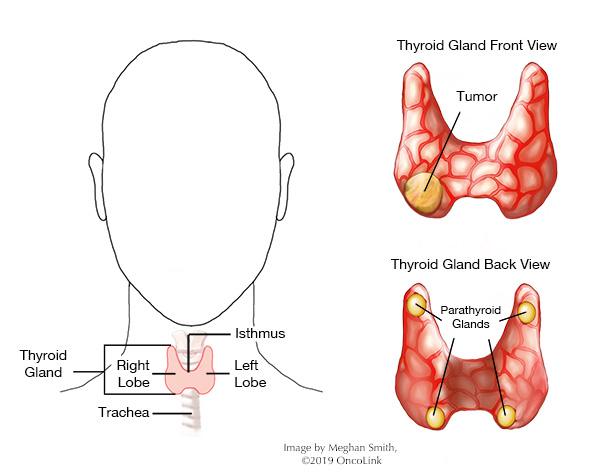
When there are cancer cells in your parathyroid gland, it is called parathyroid cancer. This disease is rare and affects the small, pea-sized parathyroid glands found behind the thyroid gland. The parathyroid gland makes the parathyroid hormone. This gland also stores and uses calcium in the body.
Some people are at a higher risk of parathyroid cancer than others. Those at a higher risk for parathyroid cancer are those with genetic disorders such as familial isolated hyperparathyroidism (FIHP) and multiple endocrine neoplasia type 1 (MEN1) syndrome.
Note: Malignant (cancerous) cells can look like benign (noncancerous) parathyroid adenoma which can make it hard to diagnose parathyroid cancer. Your provider will look at your symptoms, serum calcium level, parathyroid hormone levels, and tumor to diagnose your cancer.
What is staging and how is it done?
Staging is a way to find out if and how far the cancer has spread in your body. Your provider will have you get a few tests to figure out the stage of your cancer. For parathyroid cancer, these tests may be:
Physical Exam: This is a general exam to look at your body and to talk about past health issues.
Serum Markers: Blood samples may be taken to check calcium and parathyroid levels. Venous sampling may be used in which blood samples are taken from specific veins.
Imaging: Radiology tests can look inside your body to look at the cancer and determine if it has spread. These tests can include:
- CAT scan (CT scan).
- Ultrasound.
- Single Photon Emission Computed Tomography (SPECT scan).
- X-Ray.
- Magnetic resonance imaging (MRI).
- Bone Density Testing.
- Angiogram.
- Sestamibi Scan.
Other: Your healthcare team may recommend other tests to check for parathyroid cancer, including urine tests.
Parathyroid cancer spreads to other parts of the body through the tissue, lymph, and blood systems. Cancer stage determines how extensive the cancer is, how far it has spread, and what your treatment course should be.
Parathyroid cancer does not have a standard staging process. It is described as localized (in one area) or metastatic (spread to other parts of the body).
What types of surgery are used to treat parathyroid cancer?
Surgical procedures used to treat parathyroid cancers are:
En Bloc Resection: Also called a parathyroidectomy, an en bloc resection removes the whole parathyroid gland, the surrounding capsule (tissue around it), and at times the half of the thyroid that the cancer is found in, muscles, tissues, and nerves. This procedure can be done as an open procedure with an incision (surgical cut) in the neck or as a minimally invasive procedure using a fiber-optic scope (no incisions).
Tumor Debulking: As much of the tumor as possible is removed. At times the whole tumor is unable to be removed.
Metastasectomy: A metastasectomy is a procedure to remove cancer that has metastasized (spread) to other parts of the body.
With each of these surgeries, the main goal is to have “clean margins.” This means that the edges of the tissue that were removed are free of cancer cells when looked at under a microscope. Your surgeon will try to remove enough tissue so that the margins do not have cancer in them. Having these “clean margins” lowers the risk of cancer growing back (recurrence).
What are the risks of parathyroid surgery?
As with any surgery, there are risks and possible side effects. These can be:
- Bleeding.
- Cardiovascular (heart) issues, such as heart attack.
- Blood clots.
- Wound infections.
- Chest infections like pneumonia.
- Low calcium levels.
- Hypothyroidism if the thyroid gland was also removed.
- Keloid (thick scar tissue) formation.
- Numbness at the incision or under the chin that goes away.
- Lump in the throat or throat pressure that goes away.
- Incisional itching.
- Neck stiffness, tightness, pulling.
- Chest discomfort.
- Headache, ear pain, and/or congestion.
- Hoarse/weak voice and/or pitch/tone changes that goes away. Permanent hoarseness may happen in those that have injury to the recurrent laryngeal nerve (a nerve in your neck).
- Emotional changes which often get better over time, including depression, irritability, fatigue, and/or weakness.
Some people are at a higher risk for side effects and/or surgical complications. Speak with your healthcare team if you have concerns about your surgical risks and possible side effects.
What is recovery like?
Your team will decide if you need to stay in the hospital and for how long. You will be told how to care for your surgical incision before leaving the hospital. Most times you can return to normal activities within 1-2 weeks.
Your care team will talk with you about the medications you will be taking, such as those for pain and/or to treat hypothyroidism, as well as any activity restrictions you may have.
Common activity restrictions and postoperative instructions for parathyroid surgery are:
- Showering is usually allowed 48 hours following surgery. Pat the incision dry after a shower. Let the steri-strips to fall off or remove them by day 10-14.
- Avoid swimming or tub soaking for 2 weeks.
- Avoid driving until you are not taking pain medication and can turn your neck side to side, usually within 1-2 weeks following surgery.
- Due to possible temporary throat discomfort or swallowing problems, eat soft foods or easily-swallowed foods/drinks such as juice, soup, applesauce, scrambled eggs, etc.
Call your care team if you have:
- Fever or signs of an infection like chills, incisional redness, tenderness, and/or drainage. Your care team will tell you at what temperature you should call them.
- Any feelings of dizziness or if you are lightheaded.
- Shortness of breath/having a hard time breathing.
- Nausea/vomiting.
- Numbness/tingling in the hands, feet, and/or mouth.
- Muscle spasms.
How can I care for myself?
You may need a family member or friend to help you with your daily tasks until you are feeling better. It may take some time before your team tells you that it is ok to go back to your normal activity.
Be sure to take your prescribed medications as directed to prevent pain, infection and/or constipation. Call your team with any new or worsening symptoms.
There are ways to manage constipation after your surgery. You can change your diet, drink more fluids, and take over-the-counter medications. Talk with your care team before taking any medications for constipation.
Taking deep breaths and resting can help manage pain, keep your lungs healthy after anesthesia, and promote good drainage of lymphatic fluid. Try to do deep breathing and relaxation exercises a few times a day in the first week, or when you notice you are extra tense.
- Example of a relaxation exercise: While sitting, close your eyes and take 5-10 slow deep breaths. Relax your muscles. Slowly roll your head and shoulders.
This article contains general information. Please be sure to talk to your care team about your specific plan and recovery.